
I’m currently taking a short break from the blog, but encourage you to follow along on Instagram. I will be back with blog content soon. To know exactly when that happens, make sure to subscribe!
Thanks and ‘see’ you soon!


I’m currently taking a short break from the blog, but encourage you to follow along on Instagram. I will be back with blog content soon. To know exactly when that happens, make sure to subscribe!
Thanks and ‘see’ you soon!


And…I’m back! Took a nice two week break from writing the blog to focus on some other things, but I’m officially back! As such, and because I’ve been experimenting with some cooking lately, I thought I would share a little bit about COVID-19 nutrition, because we’ve all been doing a whole lotta eating at home lately…at least I know I have!
The Centers for Disease Control has a great page on ‘Food and COVID-19‘ that I reviewed for today’s post. The main takeaways are (for those tl;dr folks):
There may be a lot of people out there pushing you to buy supplements and other things during this time, but rest assured that the best way to get the best nutrition and dietary nutrients your body may need is through eating well-balanced, nutritious meals! So stay away from people tryna sell you bottles of “covid-prevention liquids, pills, or mixtures” and run to the grocery store and stock up on veggies and fruits instead. Might be cheaper too! If you do decide to take supplements like Vitamin D, for example, make sure you consult with a physician or registered dietician to determine what you need and what specific dose you need.
Some of you have asked me about edelberry. While this has not been studied in the context of COVID-19 specifically, the best advice I found was from the Andrew Weil Center for Integrative Medicine at The University of Arizona. Some evidence suggests it may ‘help boost immunity’ and possibly lengthen the duration of flu symptoms for example, though this evidence has not been rigorously tested (eg, unknown whether people who take edelberry are more likely to be healthier, younger, etc in general, or, if there is some placebo effect at play. That aside, what is cautioned with respect to edelberry is its potential contribution to the ‘cytokine storm’ we are seeing in some COVID-19 patients. The site states, “For this reason, to minimize the possibility that elderberry could aggravate the inflammatory “cytokine storm” associated with the more severe COVID-19 infections, it is recommended to stop elderberry at the first signs of infection (fever, cough, sore throat) and/or if you test positive for the virus.” Because you can test positive and NOT have any or only mild symptoms, it might be advisable to lay off the eldeberry juice or gummies.
Taking all that into consideration, we have cooked at home a lot lately, and today, sharing this salad, as it is one of my absolute favorites. You can make it with any combination or raw veggies, really, but the key if using kale, is to massage the kale with olive oil to soften it, and then squeeze some lemon over the entire salad. Sprinkle some salt and pepper on it, and voila! You have a healthy, nutrient packed salad!

Here’s another salad I love, and one that my mom has made for years. Use as a garnish, or eat alone. Made out of cactus and what is best known as ‘pico de gallo’!

I’ve also engaged the kids in cooking a lot lately. In fact, I have found that if the kids are involved, they take sooooo much pride in their cooking, that that they are more likely to eat it, especially if it’s something new like kale.
Anyway! So, after all that you want to know how to prevent getting sick with COVID-19?
Six easy things, and they don’t cost you any money! Except of course unless you don’t already have a mask. Here are some you can buy if you still don’t have any at home. Oh yeah, and eat those healthy meals as much as possible. I won’t be mad at ya if you throw some fries on the side though, because honestly, that’s how I roll. It’s called balance. 😀

First and foremost, a Happy Father’s Day to all the fathers and father figures! Today’s post is focused on reminding all the men in our lives about keeping healthy habits. Did you know that the week leading up to Father’s Day (happy day to all the Father’s out there!), is National Men’s Health Week? A week to remind us all there are easy things we can do to help all the men in our lives stay healthy.
According to the CDC, leading causes of death in the US include:
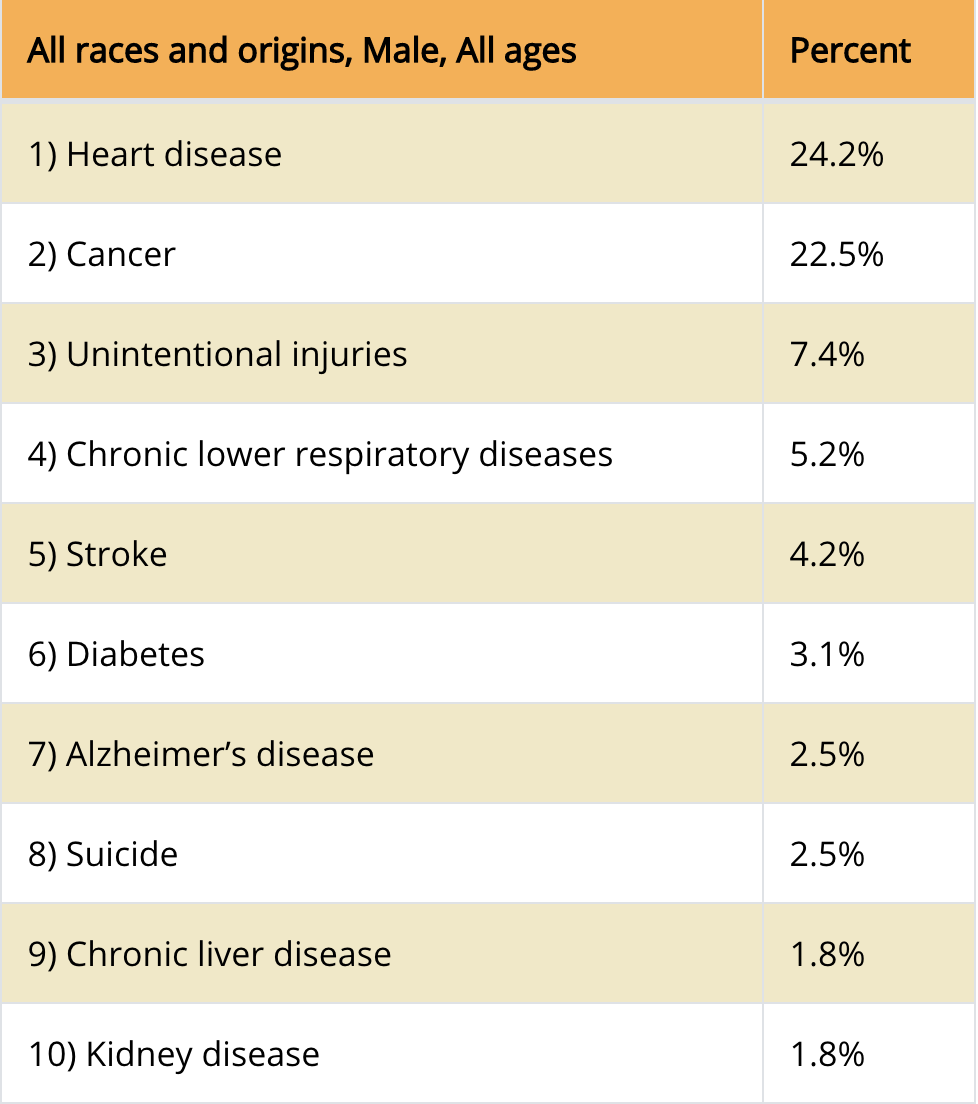
As such, here are five things to remember to ensure healthy lives for all men in our lives:
Every 40 seconds someone in the U.S. has a heart attack. If you think you or someone you know is having a heart attack call 911 immediately. Major signs of a heart attack include:
- Pain or discomfort in the jaw, neck, or back
- Feeling weak, light-headed, or faint
- Chest pain or discomfort
- Pain or discomfort in arms or shoulder
- Shortness of breath
For more information, visit the heart.org.
- Signs of depression include persistent sadness, grumpiness, feelings of hopelessness, tiredness and decreased energy, and thoughts of suicide.
- Those that suffer from depression or anxiety should seek help as early as possible. If you or someone you care about is in crisis, please seek help immediately.
- Call 911
- Visit a nearby emergency department or your health care provider’s office
- Call the toll-free, 24-hour hotline of the National Suicide Prevention Lifeline at 1-800-273-TALK (1-800-273-8255); TTY: 1-800-799-4TTY (4889) to talk to a trained counselor

